Chronic Bronchitis Treatment in Connecticut
Relief for Ongoing Cough and Breathing Changes
Chronic bronchitis is a long-term condition that causes inflammation in the airways, leading to a persistent cough and mucus production. If you are experiencing a cough that does not go away, frequent chest congestion, or ongoing changes in breathing, an evaluation may be needed.
PACT Pulmonology provides chronic bronchitis treatment in Connecticut, focusing on identifying the cause of your symptoms and managing them over time.
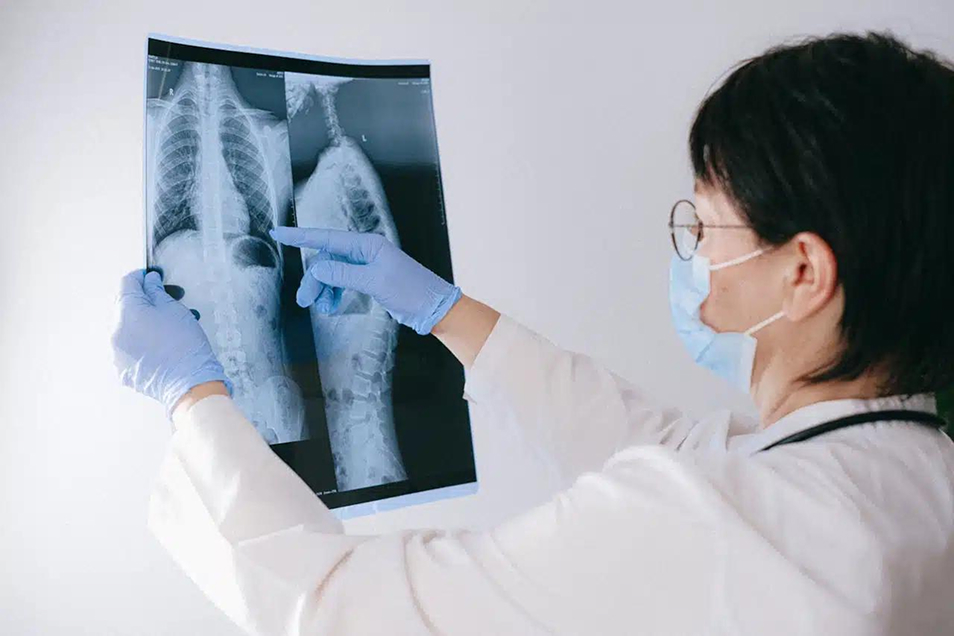
What Is Chronic Bronchitis?
Chronic bronchitis is a form of chronic obstructive pulmonary disease (COPD) that affects the airways and leads to ongoing inflammation.
It is typically defined as a productive cough lasting at least three months and recurring over time. Unlike short-term bronchitis caused by infections, chronic bronchitis is a long-term condition that requires ongoing care.
Symptoms and Causes
Chronic bronchitis symptoms are often ongoing and may become more noticeable over time.
Common Symptoms
- Persistent cough with mucus
- Shortness of breath, especially during activity
- Wheezing or chest tightness
- Frequent chest congestion
- Fatigue related to breathing changes
Common Causes and Risk Factors
- Long-term smoking or exposure to secondhand smoke
- Exposure to dust, chemicals, or air pollution
- Repeated respiratory infections
- Underlying lung conditions such as COPD
In some cases, the exact cause is not identified.
How Chronic Bronchitis Differs from Temporary Illness
Chronic bronchitis is often mistaken for a lingering cold or seasonal bronchitis, but there are key differences.
- Symptoms last for months rather than days or weeks
- Cough is persistent and produces mucus
- Symptoms tend to return or worsen over time
- Breathing changes are more consistent
If a cough continues beyond a typical illness or keeps coming back, it may be time for further evaluation.
Diagnosis and Evaluation
- Review of symptoms, medical history, and exposure risks
- Pulmonary function testing to assess airflow and lung capacity
- Imaging, such as chest X-rays, when needed
- Additional testing to rule out other respiratory conditions
These findings guide how your care is planned and monitored.
Treatment and Symptom Management
Airway-Focused Medications
Prescriptions may be used to relax airway muscles and reduce inflammation, making breathing feel less restricted.
Mucus Management Strategies
Techniques such as controlled coughing and breathing exercises may be recommended to clear mucus more effectively.
Pulmonary Rehabilitation Programs
Guided programs support stamina, breathing control, and day-to-day activity through structured exercise and education.
Reducing Exposure to Irritants
Avoiding smoke, air pollution, and workplace irritants can limit symptom triggers and reduce airway irritation.
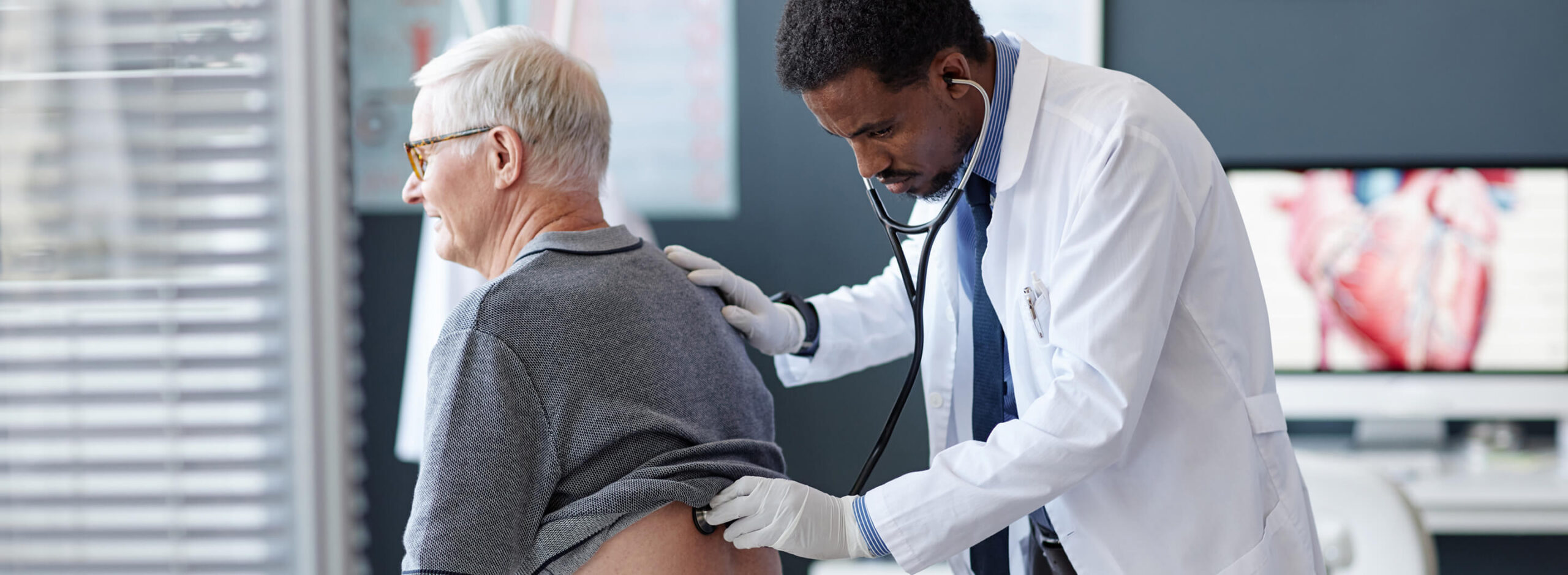
When to See a Pulmonologist
Persistent respiratory symptoms should not be ignored, especially when they affect daily activity.
You may benefit from seeing a pulmonologist if you have:
- A cough that lasts for several weeks or longer
- Ongoing mucus production or chest congestion
- Shortness of breath during routine activity
- Frequent respiratory infections or flare-ups
Specialty care allows for a more detailed evaluation and a clearer plan for managing symptoms.
Request Chronic Bronchitis Care
Connect with a PACT provider to review your symptoms and discuss next steps.
Frequently Asked Questions
How long does chronic bronchitis last?
Chronic bronchitis is a long-term condition. Symptoms may be ongoing or come and go, but they tend to persist for months or return over time.
What makes chronic bronchitis worse?
Exposure to smoke, air pollution, dust, and respiratory infections can aggravate symptoms and lead to flare-ups.
Is chronic bronchitis the same as COPD?
Chronic bronchitis is one type of COPD. Not everyone with COPD has chronic bronchitis, but it is one of the conditions within that group.
Can chronic bronchitis improve with treatment?
Treatment focuses on reducing symptoms and improving breathing. While the condition does not go away, symptoms can become more manageable with ongoing care.
Do I need testing for chronic bronchitis?
Testing may be recommended to evaluate lung function and rule out other conditions. This often includes pulmonary function testing or imaging.
